Heart treatment has changed dramatically over the last two decades. Earlier, many cardiac conditions required major open-heart surgery, long hospital stays, and extended recovery periods. Today, advancements in interventional cardiology have transformed the way doctors diagnose and treat heart diseases with minimally invasive procedures.
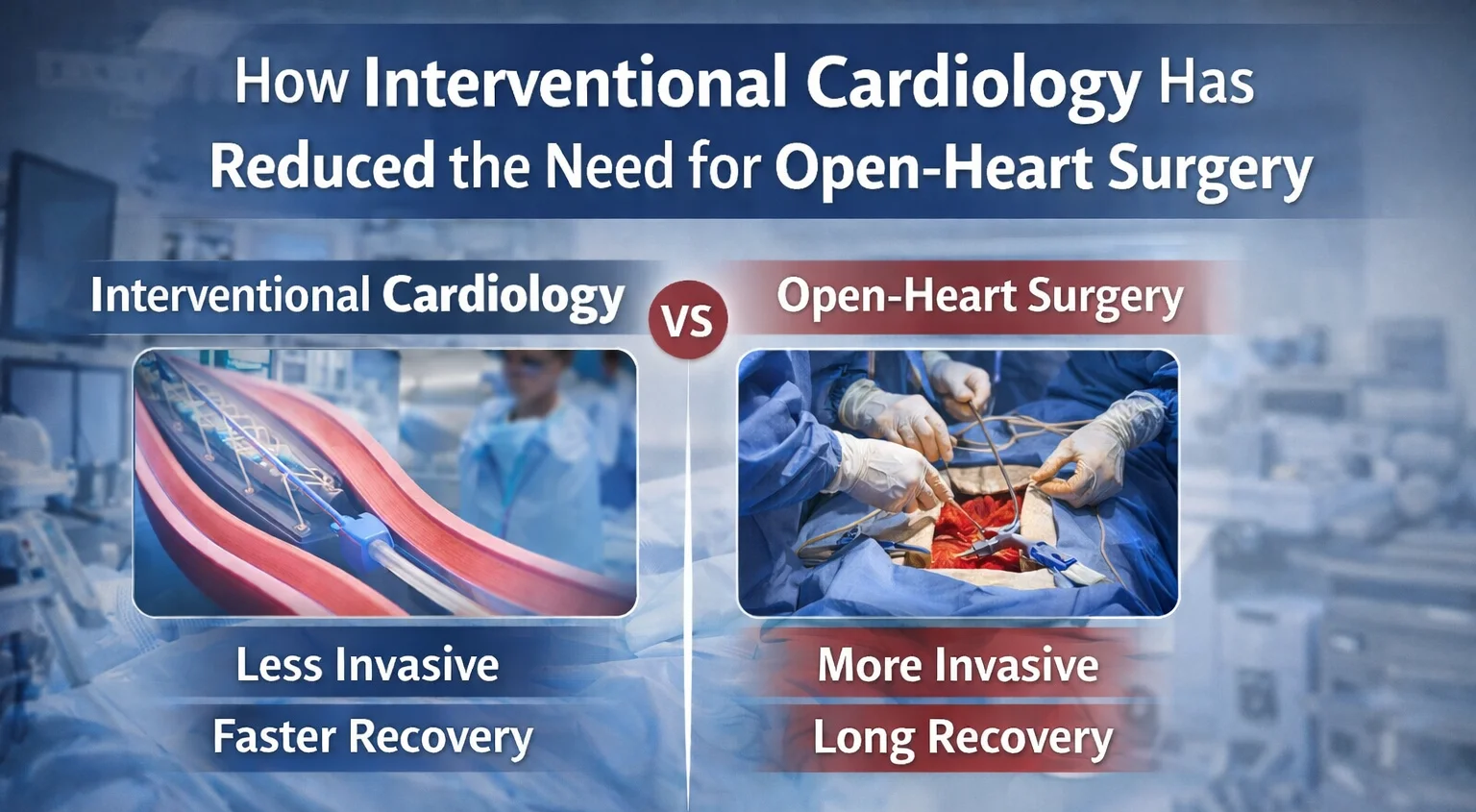
Interventional cardiology focuses on treating heart conditions using catheters, balloons, stents, and other advanced devices inserted through small blood vessels instead of opening the chest. These modern techniques have significantly reduced the need for traditional open-heart surgery for many patients.
Interventional cardiology is a specialized branch of cardiology that uses minimally invasive procedures to diagnose and treat cardiovascular diseases. Instead of performing large surgical incisions, doctors use thin tubes called catheters to access the heart through arteries in the wrist or groin.
Because these treatments are less invasive, patients often experience faster recovery, reduced pain, and fewer complications compared to open-heart surgery.
Before the development of advanced interventional procedures, open-heart surgery was considered the standard treatment for severe heart problems. Conditions like blocked arteries or damaged heart valves required surgeons to open the chest and temporarily stop the heart during surgery.
Although open-heart surgery remains essential in some complex cases, it comes with challenges such as:
With the rise of minimally invasive heart procedures, many patients can now avoid these challenges.
One of the biggest breakthroughs in interventional cardiology is coronary angioplasty. In this procedure, a small balloon is used to open blocked arteries, and a stent is placed to maintain blood flow.
Earlier, patients with blocked arteries often required coronary artery bypass grafting (CABG), a major open-heart surgery. Today, many blockages can be treated successfully through angioplasty.
Transcatheter Aortic Valve Implantation (TAVI) or Transcatheter Aortic Valve Replacement (TAVR) has revolutionized the treatment of severe aortic stenosis.
Previously, elderly or high-risk patients needed open-heart valve replacement surgery. Now, doctors can replace the diseased valve using a catheter-based approach without opening the chest.
TAVI has become a preferred treatment option for many patients worldwide.
Mitral valve leakage once required surgical repair or replacement. With modern interventional techniques like MitraClip therapy, doctors can repair the valve through a catheter-based procedure.
This treatment is especially beneficial for patients who are not ideal candidates for open-heart surgery due to age or other medical conditions.
Interventional cardiology also helps treat congenital heart defects such as:
These conditions can often be corrected using closure devices delivered through catheters, eliminating the need for open-heart procedures in many cases.
allow cardiologists to perform procedures with greater precision and safety.
Improved technology has increased the success rates of minimally invasive heart treatments and further reduced dependence on traditional surgery.
Most interventional procedures require only small punctures instead of large incisions. Patients usually recover within days rather than weeks or months.
Minimally invasive techniques cause less tissue damage, resulting in less pain and minimal scarring.
especially in carefully selected patients.
Many patients are discharged within 24 to 72 hours after the procedure.
Patients can return to normal activities faster and enjoy improved heart function with less physical stress.
Yes. Open-heart surgery still plays a crucial role in treating certain complex heart conditions. Some patients may require surgery for:
The choice between interventional cardiology and surgery depends on:
A heart specialist carefully evaluates each case before recommending the most appropriate treatment.
Interventional cardiology is particularly beneficial for:
Consulting an experienced interventional cardiologist is important to determine the best treatment approach.
The field of interventional cardiology continues to evolve rapidly. New technologies and robotic-assisted procedures are making treatments safer and more effective.
Future advancements may further reduce the need for open-heart surgery while improving patient outcomes and long-term heart health.
Interventional cardiology has transformed modern heart care by offering minimally invasive alternatives to traditional open-heart surgery. Procedures such as angioplasty, TAVI, MitraClip, and device closures have helped countless patients receive effective treatment with less pain, shorter recovery, and lower risk.
While open-heart surgery remains essential for certain complex cases, interventional cardiology has significantly reduced its necessity for many heart conditions. Early diagnosis, advanced technology, and expert cardiac care continue to improve the future of cardiovascular treatment.